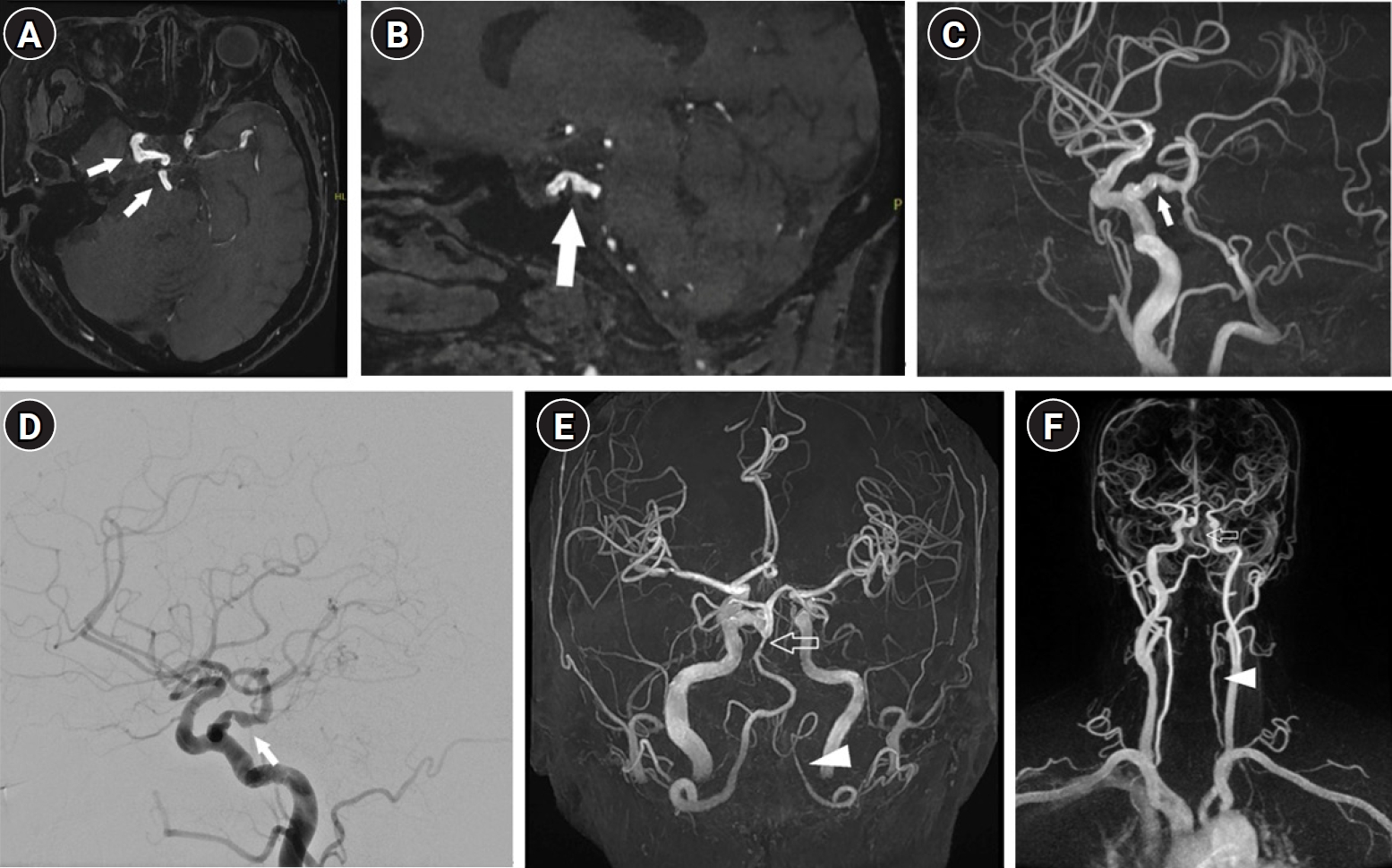
 , Boeun Lee
, Boeun Lee
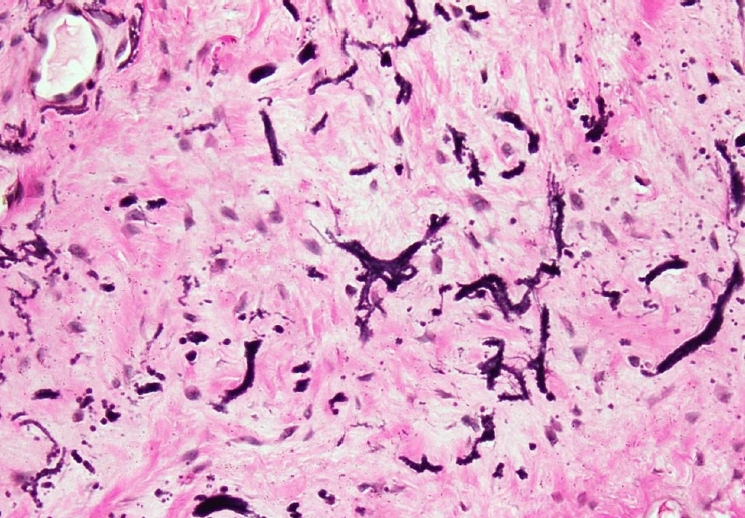
 , Muhammed Said Aydin
, Muhammed Said Aydin , Gokay Ozler
, Gokay Ozler , Onur Ozvurmaz
, Onur Ozvurmaz , Celal Kahraman
, Celal Kahraman , Hasan Can Çoban
, Hasan Can Çoban , Mert Kahraman
, Mert Kahraman , Ozan Dağdelen
, Ozan Dağdelen
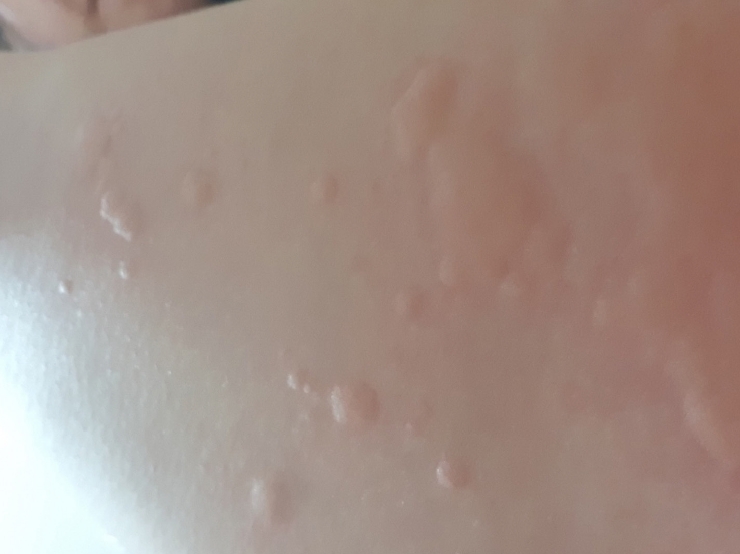
 , Dae Hwan Kim
, Dae Hwan Kim , Yunyoung Nam
, Yunyoung Nam , Jeong Eun Sohn
, Jeong Eun Sohn , Geunwoong Noh
, Geunwoong Noh
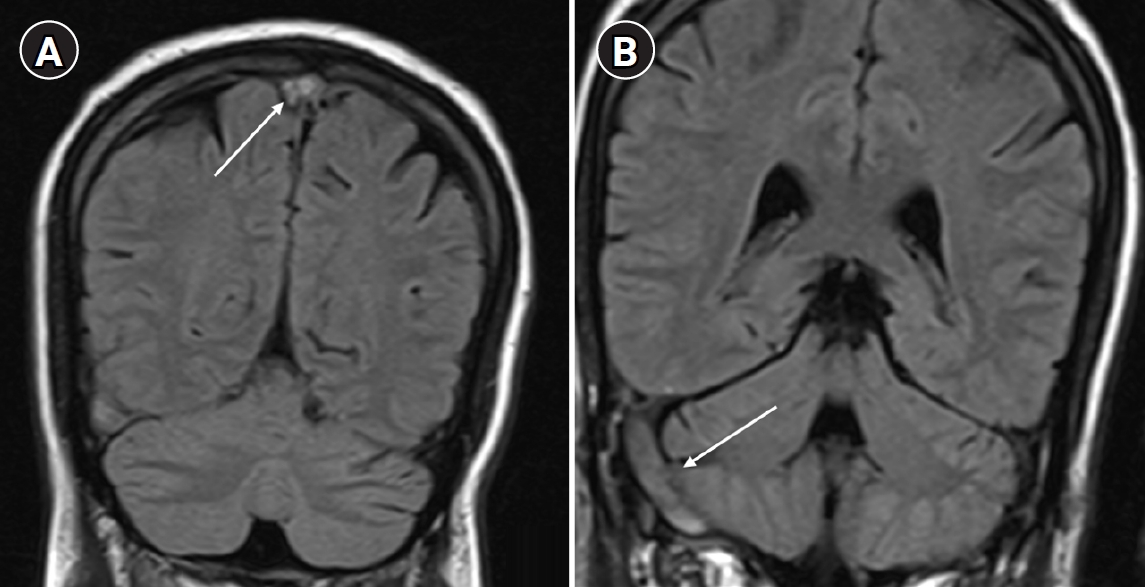
 , Viswanathan Pandurangan, Devasena Srinivasan
, Viswanathan Pandurangan, Devasena Srinivasan 
 , So Young Lee
, So Young Lee
Citations

 , Abdulraheem Almokhtar
, Abdulraheem Almokhtar , Hashem Bukhary
, Hashem Bukhary , Raed Sharaf
, Raed Sharaf , Khalid Alhomayani
, Khalid Alhomayani

